Trauma and Orthopaedics
The Impact of Obesity on Bone and Joint Health
Patient Information Leaflet
The impact of obesity on bone and joint health
- Obesity is one of the most common diseases that adversely affects bone and joint health. The Health Survey for England 2021 estimated that 25.9 per cent of adults in England are obese and a further 37.9 per cent are overweight but not obese. Obesity is usually defined as having a body mass index (BMI) of 30 or more. A BMI between 25-30 is classed as overweight.
- Obesity contributes to soft tissue damage and osteoarthritis – a progressive wear and tear disease of the joints.
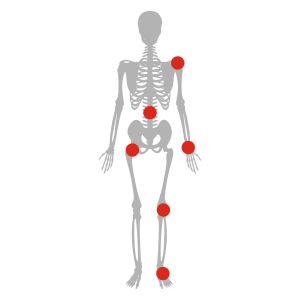
Shoulder: Lower functional outcomes following rotator cuff injuries and repair.
Spine: Higher rates of hardware failure, complications and infections.
Hand: A direct decrease in hand grip strength.
Hip and Knee: Significantly higher rates of complication and hardware failure after total joint arthroplasty [TJA]. However, postoperative function greatly improves after surgery in individuals with obesity.
Foot and Ankle: Excess weight can cause chronic overuse disorders of the foot and ankle like ‘flat foot’ which can lead to plantar fasciitis, Achilles tendonitis and foot and ankle pain.
- Each pound (lb) of body weight places four to six pounds of pressure on each knee joint. Individuals with obesity are 20 times more likely to need a knee replacement than those who are not overweight.
- Obesity is also linked to diabetes, heart disease, liver disease, certain cancers, and psychiatric disorders.
- Complications around the time of surgery that may result from obesity include poor wound healing, infections, blood clots, blood loss, increased total operative time and length of hospital stay.
*From the 2015 AAOS Position Statement on the Impact of Obesity on Bone and Joint Health; Modified 2021
Weight reduction strategies
- Calorie reduction: a well-balanced calorie restricted diet is the most prescribed method for weight loss. A calorie reduction of 500 to 1000 kcals from a typical daily consumption should be adequate for fat stores to be used and in meeting daily energy requirements. This typically totals 1200 to 1800 kcals of daily calorie intake.
- Nutritional quality: weight loss is promoted through diets rich in vegetables, fruits, lean proteins and whole grains. When looking at a plate, half of the plate should be composed of non-starchy vegetables and the other half should be split equally to include a lean protein and a whole food grain item.

- Exercise: consistent exercise is a beneficial addition to a restricted diet in terms of weight loss and overall health. Aquatic exercise (swimming / aqua aerobics etc) and resistance training are all beneficial.
- Lifestyle: lifestyle changes along with community support is effective, especially when inspiration and accountability are included. Search for local weight loss community support groups in your area.
- Weight gain prevention: the following habits have helped to promote weight maintenance – eating breakfast daily, weighing in at least weekly, restricting television to less than 10 hours per week and exercising an average of one hour per day.
- Pharmacotherapeutics: pharmacotherapeutics (medications) have been shown to help patients lose more weight and keep it off longer. Medications must be taken long term like any other chronic disease to be effective.
- Bariatric surgery: bariatric surgery is an effective method for weight loss in patients with obesity who have a BMI greater than 35 with a weight-related comorbidity, or a BMI greater than 40 who have failed conservative weight loss efforts.
Helpful nutrition and weight loss links:
- Healthy Eating Plate: https://www.hsph.harvard.edu/nutritionsource/healthy-eating-plate/
- The National Weight Control Registry: http://www.nwcr.ws/
- Slimming World: https://www.slimmingworld.co.uk/
- Weight Watchers: https://www.weightwatchers.com/uk/
Helpful Smartphone apps:
- Garmin
- Samsung Health
- FitBit
- Apple Health
- MapMyRun
- MyFitnessPal: https://www.myfitnesspal.com/
- Lose It!: https://www.loseit.com/
- RP Diet Coach App: https://www.rpdiet.app/
*Many smartphone applications exist, and this list is not exhaustive. We have no endorsements with the companies listed above. Users should browse the many options at their own discretion. We make no guarantees. Individual results may vary.
If you have any questions, or if there is anything you do not understand, please contact the Russells Hall Hospital switchboard number on 01384 456111 and ask for the relevant department who issued this leaflet.
If you have any feedback on this patient information leaflet please email dgft.patient.information@nhs.net
This leaflet can be made available in large print, audio version and in other languages, please call 0800 073 0510.
Originator: F Chaudhry. Date originated: January 2023. Review due: October 2028. Version: 2. DGH ref.: DGH/PIL/02191.
